By Linda Meixner, Development Director, Woodley House
Woodley House is a community-based organization dedicated to helping men and women struggling with persistent mental illness live full and healthy lives with dignity. We offer the opportunity to heal within a safe and comforting residential community as they work toward recovery and reclaiming their lives.
Woodley House serves over 300 adult men and women each year who have been diagnosed with severe mental illness, many of whom are lower-income and at risk of becoming homeless. We provide a residential housing program and supportive services needed to achieve greater independence. Mental illness cuts across all socio-economic and ethnic groups, but is often ignored or overlooked due to the entrenched stigma surrounding it. Woodley House exists to help our residents attain the stability and life skills needed to recover and reintegrate into their community.

One in five of us will experience a mental health issue in the coming year — this affects us all. For some, this may be a temporary period of intense anxiety or depression, while for others, the reality will be much more severe and long-lasting. When your mind is working against you, it can be very isolating and the challenges of just living each day can be truly overwhelming.
Woodley House takes a whole-person approach, viewing our residents as individuals, not simply as clients with a diagnosis. We know that having a home with a welcoming, family-like environment is critical to achieving stability and hope for the future.

We offer a range of housing, from short-term crisis stabilization, to longer-term group homes and finally, shared apartments throughout the city as part of our Supported Independent Living Program, so we are there – through each step of their journey to recovery. But simply providing a home, while very important, isn’t enough. People need to have the ability to maintain that home to be truly successful.
Woodley House offers personalized support through our Life Skills Trainers who meet with each resident, both individually and in groups, multiple times per week. They work together on issues particular to that resident, from basic hygiene and room/apartment maintenance, to budgeting, nutrition, communication skills and job readiness. We work with, not for, our residents and this very personal approach has proved successful for nearly 60 years.
Celebrating our 60th anniversary in 2018, we have succeeded by offering essential, life-changing services for a very vulnerable population.
- “Success” for Woodley House means the ability to continue to provide our residential and supportive services long into the future for the men and women in the District who struggle each day with mental illness.
- “Success” is also when our residents, helped by the daily support of Woodley House, overcome the vagaries of their mental illness and “graduate” to a bright, secure future by achieving and maintaining their stability in the most independent lives in the community that they can manage.
- Many residents move on to greater independence in shared, semi-independent apartments, or to total independence. For others, their best success is achieved in a more structured environment helping them maintain a stable, full life.
Woodley House serves the full spectrum of people needing our help and we applaud them all.

A basic tenet of Woodley House is that each person is viewed as an individual and will be treated with the dignity and respect that we all deserve. The goals of one resident might differ from those of another, but they all share the desire to remain stable and work toward fuller, more independent lives. Our residents come to us in varying stages of recovery, so success for some might mean appreciating a stable, caring home after years on the streets, while others may be further along on their journey, and a new job might be the highlight of their year.
One resident of Holly House recently got a part-time custodial job at Howard University and is so excited that she is always waiting by the curb at 6:30 in the morning for the van that picks her up at 7 to ensure that she won?t be late! Success for our residents is individual, but all share the goal of learning to live with their symptoms so that they can achieve the fullest, most productive life possible.
Woodley House has been serving our community for nearly 60 years, but has remained a secret to far too many over the years. We welcome the opportunity to introduce ourselves and share the critical role we play to those who turn to us each year. For more information about Woodley House, please contact development director, Linda Meixner lmeixner@woodleyhouse.org to arrange a tour or simply to find out a bit more about our program. Donations are ALWAYS welcome and can be made online at www.woodleyhouse.org or mailed to: Woodley House, Inc. 6856 Eastern Avenue, NW – # 300 Washington, DC 20012.






 May is Mental Health Awareness Month, and today we’re getting a glimpse into the important work of Arlington Free Clinic, and its Behavioral Health program. Arlington Free Clinic provides free high-quality medical care to low-income, uninsured Arlington County adults. In the following piece, AFC’s Behavioral Health Program Manager, Jyl Pomeroy RN, discusses some of the health struggles that immigrants face as a result of their experiences before, during, and after arriving in the United States, and how AFC’s Behavioral Health Program offers its support.
May is Mental Health Awareness Month, and today we’re getting a glimpse into the important work of Arlington Free Clinic, and its Behavioral Health program. Arlington Free Clinic provides free high-quality medical care to low-income, uninsured Arlington County adults. In the following piece, AFC’s Behavioral Health Program Manager, Jyl Pomeroy RN, discusses some of the health struggles that immigrants face as a result of their experiences before, during, and after arriving in the United States, and how AFC’s Behavioral Health Program offers its support.
 Each year, more than 40 million Americans experience mental illness, and 50 percent of Americans will meet the criteria for a diagnosable mental health condition sometime in their life (with half of those people developing conditions by the age of 14)*.
Each year, more than 40 million Americans experience mental illness, and 50 percent of Americans will meet the criteria for a diagnosable mental health condition sometime in their life (with half of those people developing conditions by the age of 14)*.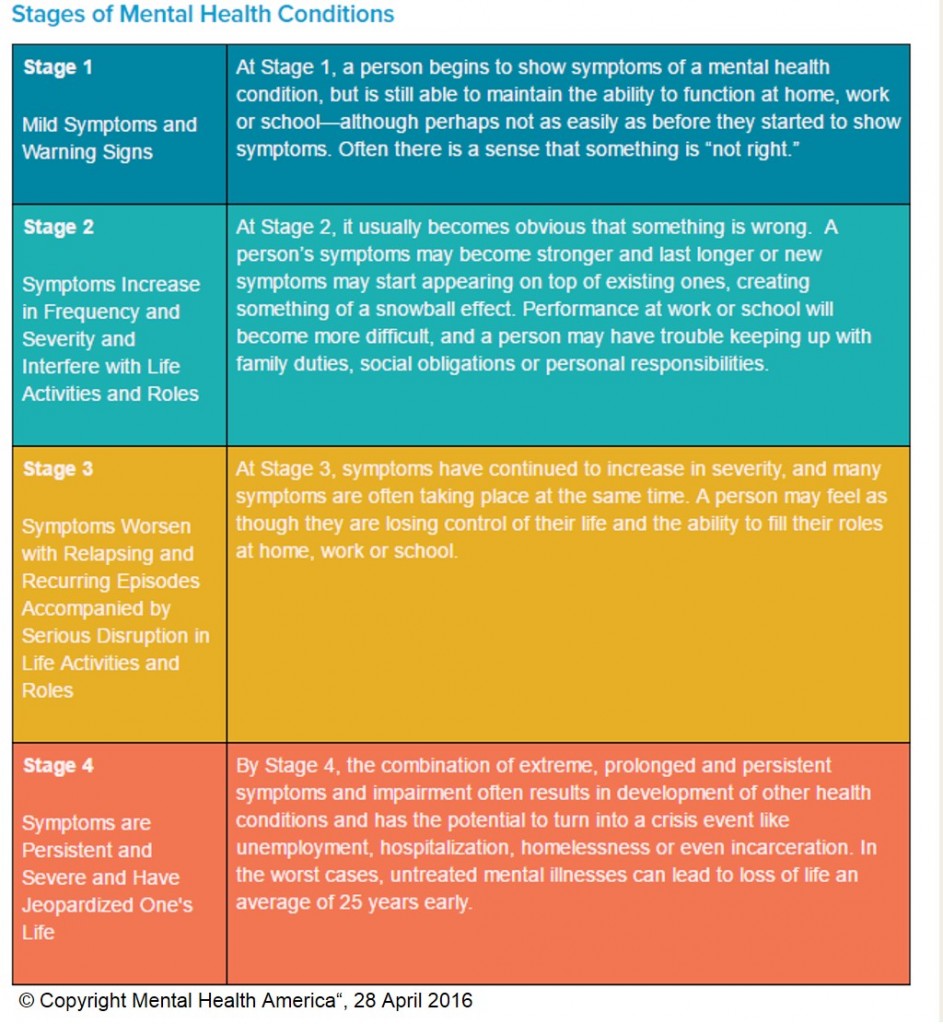

 Ascensions Community Services, Inc.
Ascensions Community Services, Inc. Wendt Center for Loss and Healing
Wendt Center for Loss and Healing
